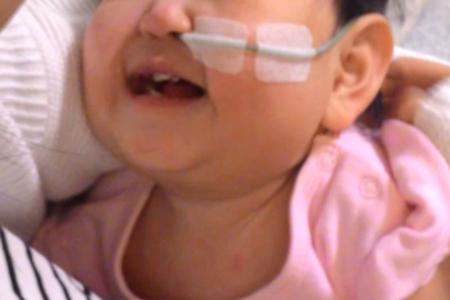
Toddler with rare stomach condition needs surgery in US
Toddler needs $1.7 million to treat rare stomach condition. Mum says: "I want to give her a chance"
Behind her chubby cheeks and beguiling smile lie medical problems that would make an adult shudder.
Little Xie Yujia, just 21 months old, was born with long-gap oesophageal atresia, which means her food pipe is not connected to her stomach.
Along with the rare congenital defect - it strikes one in 5,000 in the West - she suffers from other anomalies like a heartbeat rhythm disorder, global development delay and poor vision in both eyes.
But her mother, Ms Jamie Chua, remains optimistic about Yujia's health.
"This time round, we are in a way fortunate because she's alive and kicking," said the 30-year-old.
"It's a very magical feeling and I love kids a lot. To me, it's already a blessing that my second (pregnancy) made it."
She said that her first pregnancy in 2011 ended in an abortion after doctors discovered her foetus was not developing properly and would be stillborn.
Speaking to The New Paper last week, the freelance model and housewife said the warning signs about Yujia started in the middle of her pregnancy.
Her fifth ultrasound scan revealed "many scary things" about her child's brain and heart, but nothing related to the oesophagus.
"At my last scan, I was told that maybe there was a blockage in the food pipe. But I got the impression that it wasn't anything serious," Madam Chua said.
"To us, this is already a very good thing, compared to the first one. I thought that as long as she can survive or develop, I want to give her a chance."
A day after Yujia was born in September 2013, doctors tried to operate on her but realised that the gap between the two ends of her oesophagus was too wide.
The interim measure was to create a peg in Yujia's stomach and feed her through a tube.
For the next few months, she stayed in the hospital, fighting infections and going for regular gap assessment check-ups. She also had to be operated on following a retinal detachment in her right eye.
In February last year, the doctors said Yujia was finally ready to be operated on for her oesophageal atresia.
After her oesophagus was joined to her stomach, the toddler started going for her dilatation sessions, a process to stretch and widen the narrowing of the oesophagus.
But four months later, a complication developed.
Doctors found a hole in the toddler's oesophagus hours after her second dilatation session.
"We knew there was this risk but we didn't expect it to happen because it had not happened before," Madam Chua said, adding that she was "crying like crazy" while trying to find out what had gone wrong.
Gastric juices started leaking into Yujia's lungs, causing them to collapse.
For the next 43 days, Madam Chua and her husband, an events organiser, watched their baby being loaded up with morphine and a cocktail of other drugs as they waited for the hole in her food pipe to heal.
"Her face was really black initially. If you saw her, you would wonder if she would make it.
"The doctors couldn't give me an answer. They just told me her oxygen saturation looked okay and left," she said.
The wound has since closed, but the rest of the oesophagus is now scarred, leaving just a pinhole-size passage.
Madam Chua said: "Even though the oesophagus is now connected, how can anything pass through that pipe?"
That incident made the couple think long and hard about treatment options for Yujia.
"We have two options - to put her through another round of dilatation (in Singapore), which had failed previously, or to go for surgery again (overseas) to reconstruct everything.
"It took us really long to decide (on the latter). If the same thing happens to her after a round of dilatation, she would be worse off," she said.
Madam Chua tried contacting hospitals in the region - in Taiwan, Indonesia and Malaysia - but had no luck. Her research then led her to Boston Children's Hospital in the US. It has a treatment programme specially designed for children with Yujia's condition.
Among all the types of the condition, long-gap oesophageal atresia is the trickiest to treat, say experts here.
Madam Chua spoke to the hospital's doctors who are confident they can help Yujia. If the surgery to reconstruct her oesophagus is successful, she would be able to eat normally, or at the very least, be able to swallow her saliva.
RAISE MONEY
The problem is the cost - about US$1.3 million (S$1.7 million). Madam Chua has so far raised about US$390,000 through two crowdfunding campaigns.
Till she can afford the operation, she is making sure her little girl is living as comfortably as possible.
The toddler continues to be tube-fed through a peg in the stomach with milk mixed with porridge water for more nutrition.
Every two to three hours, Madam Chua has to pump saliva out of Yujia's mouth - something the toddler hates - to prevent her from choking on her saliva.
At 21 months, Yujia can barely talk. She responds to music and has started grabbing things with her hands. Those are things that other babies would have learnt before turning one, but Madam Chua is content to celebrate the little milestones.
"For us, we just want her to be physically comfortable... everything else will just come naturally, probably slower.
"But it doesn't matter at all," she said as she stroked Yujia's hair.
WHAT IS OESOPHAGEAL ATRESIA?
Oesophageal atresia is a rare birth defect in which a baby is born without part of the oesophagus, leaving a gap between it and the stomach.
For 21-month-old Xie Yujia, there is a huge gap between the two ends of her oesophagus, a type known as long-gap oesophageal atresia.
Dr Anselm Lee, a paediatrician in private practice, said there is not much information about this congenital defect in Asia.
But he said figures show that it affects one in 5,000 live births in the West.
The only way to treat it is to connect the blunt end of the oesophagus to the stomach.
"From the anatomical point of view, oesophageal atresia is a correctable condition, but the functional aspect of the oesophagus may not be 100 per cent restored," Dr Lee said.
Paediatric surgeons contacted by The New Paper said long-gap oesophageal atresia is the trickiest to treat among all types of the condition.
They declined to comment further on the surgical aspects in treating long gap oesophageal atresia.
Dr Russell Jennings, the director of the Esophageal Atresia Treatment Program at Boston Children's Hospital, said on the hospital's YouTube channel that some of the treatment options include pulling the stomach higher up to join the oesophagus to it, or to put something as a conduit between the two ends of the oesophagus.
A third option, called the Foker process, is a method practised exclusively at Boston Children's Hospital.
It involves placing small sutures in the damaged ends of the oesophagus, then adding small amounts of tension to the sutures daily.
This tension stimulates the oesophageal ends to grow longer, eventually closing the gap.
The ends are then surgically connected.
Get The New Paper on your phone with the free TNP app. Download from the Apple App Store or Google Play Store now